A number of potential bearing surfaces can be considered in a hip replacement.
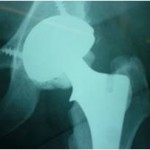
Traditionally, a high molecular weight polyethylene acetabular component has been used against a metal femoral head. This bearing has, over years, given excellent pain relief and improvement in function. There are many series in the literature that report implant survival beyond fifteen to twenty years with this bearing surface. Typically, however, in younger, more active patients, as the years progress and activity continues, the wear debris that results from this bearing can lead to a local soft tissue reaction that can, over time, be associated with loosening of the implant and subsequently with damage to the surrounding bone in a process called aseptic loosening. As detailed elsewhere in this website, this can lead to loosening and failure of the reconstruction, possibly requiring revision surgery. Indeed, if the wear is allowed to continue, the wear products and local reaction to them can result in quite considerable bone loss requiring more complex reconstruction at the time of revision.
In an attempt to improve the outcome, various changes to the materials used have been made. A technique known as ‘cross-linking’ of the polyethylene has been utilised to improve the wear characteristics. Cross-linked polyethylene has been used as a standard bearing surface over the course of the last fifteen to twenty years in my own practice. Published review and National Joint Registries data has shown very encouraging early, mid and longer-term clinical results with significantly reduced wear. This has further supported my use of highly cross-linked polyethylene with an uncemented socket as routine within my practice.
While a soft tissue reaction and resulting osteolysis (breakdown of bone) is rare with the use of cross-linked polyethylene, it has always been my practice to arrange regular ‘follow-up’ review for my patients undergoing total hip arthroplasty surgery. This would typically involve a clinical review and an x-ray review to ensure that all continues to progress well over time and with the ongoing activity. My follow-up regime is detailed elsewhere on the website.
As a combination of ongoing concerns, particularly surrounding large head metal-on-metal bearings in hip replacement surgery, and indeed with ongoing developments and improvements with more traditional bearing surfaces, the use of metal-metal bearings in hip arthroplasty surgery is now extremely rare. Beyond metal-metal hip resurfacing, I do not use metal-metal bearings within my practice.
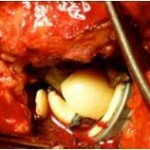
‘Ceramic-on-ceramic’ bearings have been used widely in orthopaedics for a number of years. More recent improvements in the composition and preparation of ceramics has resulted in excellent clinical results with reduced wear. This has encouraged the use of newer delta ceramic bearings. Ceramic is a harder material and has better lubrication characteristics. The resulting reduced wear rate allows the surgeon to use significantly larger diameter bearing surface options. Increased head size has been shown to reduce the rate of dislocation of the hip replacement. In addition to benefits of a reduced rate of dislocation, the wear rate of ‘ceramic-on-ceramic’ bearings is considerably lower than any of the other bearing surfaces that have been used in hip surgery.
One of the concerns that has been raised with ceramic bearings has been the fact that the material is slightly brittle. Historically, mostly with previous materials, there have been situations in which the ceramic femoral head or ceramic liner used has failed. Unfortunately, a number of the ceramic liners that have failed have been implanted in suboptimal alignment or mal-positioned with respect to the shell. Similarly, the vast majority of the ceramic heads that failed were made of older materials.
More recent developments in ceramic technology and particularly the introduction of ‘delta’ ceramic, have reduced the rate of femoral head fracture enormously. Similarly, an understanding of just how important it is that ceramic bearings are perfectly aligned and that the ceramic liners are perfectly positioned inside the uncemented shell has led to reduced concern of ceramic bearing failure.
One other concern that has been identified relating particularly to ceramic-ceramic bearings has been abnormal noise from that bearing and specifically what has been termed a ‘ceramic squeak’. This is a rare problem and has been associated with a particular implant that I have not used in large numbers within my practice. Our understanding of the aetiology of this squeak has improved significantly over recent years. As already detailed, implant squeak can occur much more commonly in some implants than others and indeed ceramic-ceramic squeak is more common when the implant has perhaps been suboptimally positioned, though not solely so.
Many well-functioning joint replacements will result in very intermittent noises and perhaps further research is required as to why this occurs. Infrequent and intermittent noises in their own right do not indicate imminent failure of a hip replacement but certainly if a patient does experience this, they should return to their orthopaedic surgeon for further evaluation to exclude any significant concern.
Unfortunately, in some very rare cases, the squeak associated with ceramic-ceramic has been significant and indeed on occasion has been intrusive and disconcerting. As detailed above, many of these cases have been related to a particular implant and to suboptimal positioning of the implant. In that circumstance the squeak has required revision of the hip replacement. I have not had to revise a hip replacement that I have inserted purely for this concern.
Theoretically, therefore, the overall effect of a ‘ceramic-ceramic’ bearing has been a better, safer range of movement with the ability to use a relatively large head size and with reduced wear rate.
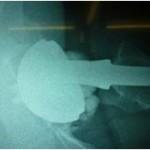
The theoretical benefits of ceramic bearings have been behind the development of a ‘ceramic-ceramic’ version of the hip resurfacing procedure. For a significant number of years now, I have been part of the design team for the MatOrtho ReCerf® device. Having been part of an international group, alongside Koen DeSmet (Ghent), Paul Beaule (Ottowa) and Bill Walter (Sydney), the group have collectively performed the earliest implantations worldwide. An initial clinical evaluation of the component is ongoing as detailed elsewhere on this website.