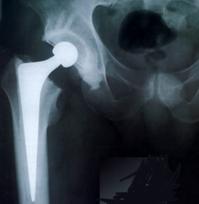
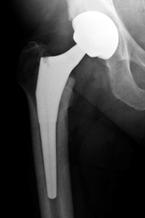
Total hip replacement involves dividing the neck of the femur to remove the very proximal part of the bone (the femur) including the damaged femoral head. This allows the surgeon to implant a metal stem into the femur.
Subsequently, the damaged articular cartilage in the socket (the acetabulum) is removed, allowing a new socket to be implanted. A round ceramic or metal femoral head is inserted onto the top of the femoral stem and a polyethylene or ceramic liner into the metal acetabular socket. Thus, a new artificial ‘ball and socket’-type bearing surface is created. (The various components involved are shown and explained within the website.)
There are various techniques and options, from the point of view of implant fixation and bearing surface, that can be used in hip replacement. This gives the surgeon a variety of options that can be used according to the patient’s age, bone quality and required activity levels at work, rest and indeed at ‘play’. There might also be underlying medical issues which can influence the surgeon’s choice of fixation technique and bearing surface options in an attempt to reduce any associated risk.
All options should be considered to ensure that the best and most reliable technique is used to provide a joint replacement. As such, the technical aspects of the procedure are essentially tailored to an individual patient’s anatomy, clinical function and to their desired level of activity post-reconstruction.
These options should be discussed around the time that a decision is taken to proceed with joint replacement surgery in advance of the surgery itself.
The results of hip replacement surgery are extremely reliable. Patients are expected to return to a very good level of function with good range of movement and excellent pain relief following the procedure.
As a specialist and experienced hip surgeon, performing around 300 to 400 primary hip operations each year, I have had a large exposure to a number of different pathologies and clinical situations in my practice over many years. This allows me to discuss an individual’s clinical situation and make informed decisions relating to what method I would plan how hip replacement can be effected most safely and reliably, aiming to return my patients to their desired level of activity. Many of my patients have a more complicated underlying situation. I feel that the experience I have gained from my extensive practice allows me to provide the best outcomes possible for those under my care.
I have always worked hard to ensure that my practice in primary hip surgery is evidence-based and as ‘up to date’ as I can make it. I consider all variables in exposure, fixation, bearing surface and rehabilitation to optimise my patients’ progress through their important surgery.
The outcomes from my work, including revision rates of patients I have operated on, can be seen within the extensive NJR database via the link in the Profile section of this website. I have always been very proud of my low revision rates following primary hip surgery, demonstrated objectively within that dataset, despite the complexity of many of the hip operations I perform.
The surgical procedure itself, including intraoperative images, is demonstrated elsewhere on this website.