There are a number of reasons why hip replacements fail and require revision surgery. Sometimes the cause of failure is more obvious than others. Around 90,000 primary hip replacements are performed in the UK each year. The number of revision procedures performed is much smaller at around 7,000. Often revision can be performed with relatively straightforward procedures. As the situation at the time revision surgery is needed becomes more complicated, particularly at second, third or fourth time surgery, this can be a major challenge. In this circumstance the surgery should be undertaken by an experienced and specialist hip revision surgeon.
The reasons for which revision might be required and the procedures that might be considered are described and illustrated in more detail below.
Wear

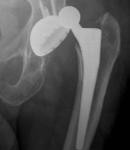
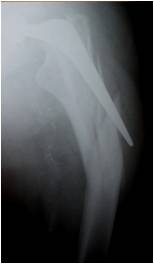
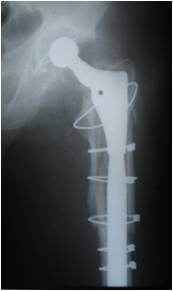
Today, the most common reason for failure of a hip replacement is loosening of the components in the absence of infection, so-called “aseptic loosening”. The most common underlying cause for this is wear of the bearing surface. Over time, with increased activity as the bearing surface head and socket move against each other, wear can occur. This wear process results in tiny particles of debris. In some circumstances a physiological response to this debris results in a soft tissue reaction around the implant which can, over years, interfere with the way the cement or indeed the implant itself is bonded to bone. If this is allowed to progress, the process can result in loosening of the implant.
Whilst this process may be asymptomatic initially, it can often be picked up on x-ray. This is one of the reasons why follow-up after total joint replacement is important. A routine x-ray, years after surgery, can identify any such concern early and initiate closer monitoring. The important decision to be taken is to intervene sufficiently early to avoid the process developing and causing bone loss around the components which can complicate revision surgery. Thankfully, more modern bearing surfaces, typically a ceramic or metal head on a crosslinked polyethylene liner, are very much more hard- wearing and have excellent longevity. We would, therefore, expect frequency of requiring revision for wear to decrease.
Infection
Despite ongoing improvements in perioperative care, surgical technique and implant design, infection remains a devastating complication for our patients. Thankfully it is rare. Infection is a concern I take very seriously. I work hard on preventing infection. My own incidence of infection after both primary and revision hip arthroplasty surgery has always been very much lower than would be expected, despite the complexity of the work I am asked to do.
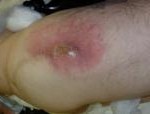
The most common time for infection to occur is acutely following surgery although infection can occur later. Most commonly the infective organism is introduced at the initial surgery. That is why careful surgery alongside fastidious preoperative screening for infection or high risk situations is important. When infection occurs acutely after surgery it is often obvious and will need urgent assessment and treatment. Any concerns with redness or discharge from around a hip scar should be seen and assessed urgently, ideally by the surgeon involved. This is also discussed in the section describing what to look out for after surgery elsewhere in my website.
Unfortunately, infection around the implant (PJI) can also arise as a consequence of concern elsewhere in the body such as chest infection, urinary tract infection, skin infection or dental sepsis. Bacteria present in the blood stream can settle onto our implant resulting in a deep infection. This can occur at any time, even years after index surgery. In this circumstance the patient is likely to experience pain and reduced function in the hip replacement but, rarely, this can result in more systemic effects with the patient becoming very unwell. While often the hip scar itself remains healed over, this can also be associated with redness in the wound area and sometimes even a discharge. Infection is investigated with blood tests and sometimes an aspiration of the joint, frequently under an anaesthetic. Certain x-rays and scans can also be helpful to diagnose infection.
Instability and dislocation
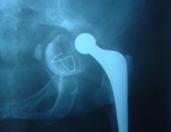
Another common cause of failure in hip replacement is instability or dislocation. Dislocation occurs when the ball comes out of the socket. Unfortunately, this is a major concern and no surgeon should underestimate the pain and distress this complication can cause our patients. Once a hip replacement has dislocated, it is unlikely to correct itself and will very likely need a procedure, likely a manipulation of the hip under an anaesthetic, to reduce the bearing.
It is not uncommon for patients to experience a sensation of movement, sometimes a ‘click’ in the hip, particularly early after surgery. This is not always a concern and will often settle as rehabilitation continues. Beyond a frank dislocation, patients can also experience more troublesome symptoms if the hip partially dislodges or ‘subluxes’. This can occur if the hip is put into a position of risk or can occur if the implants are not perfectly orientated.
Achieving the perfect orientation of the bearing surface in a hip replacement is a very important part of the surgical procedure. Many different techniques have been described and tried over years with more recent use of pre and perioperative computer planning, surgical navigation and robot assistance.
Our understanding of the reasons behind instability have developed enormously in recent years. The relative risks of this dreadful concern should be considered for each and every patient individually. Specific risks and ways they can be reduced should be discussed. Different bearing surface couples, head sizes, surgical approaches and post-op regimes can be considered, dependent on those risks.
I have worked hard to ensure the risk of dislocation for patients under my care is as low as I can make it. I am experienced in all the various methods and options to reduce those risks, varying my technique and implant choice in patients with different risk profiles.
Unfortunately, but important to appreciate, dislocation is an intrinsic concern with ‘ball and socket’ hip replacement surgery. At surgery, it is critically important to ensure that the correct and most appropriate bearing surface is chosen and is correctly and accurately implanted in the most appropriate orientation for each patient. The soft tissues should be respected, repaired and well-balanced to reduce the risk of dislocation. Unfortunately, despite all the best intentions of both surgeon and patient, dislocation can still occur. While the rate of dislocation is at its highest acutely following surgery before the soft tissues heal and the capsule around the new joint forms, dislocation can occur at any stage following hip surgery.
The most common mechanism is when the patient bends the knee upwards, often to beyond 90°. The hip is specifically at risk when the knee is then turned in towards the mid-line resulting in ‘internal’ rotation of the hip which can then dislocate the hip posteriorly. If hip dislocation occurs this can be associated with disruption of the soft tissue capsule around the hip. Unfortunately, in certain circumstances, this can become a recurrent problem. If that is the case hip revision surgery might be required to deal with whatever is thought to be the underlying cause of dislocation.
Dependent on a thorough assessment and investigation of any underlying cause, the revision procedure might merely involve exchanging the bearing components in the hip replacement, changing the head and liner to increase the soft tissue tension, increasing the head size and repairing the soft tissues. A number of helpful implants, bearings and surgical techniques can facilitate this approach. Alternatively, the procedure might require revision of all the components to change the component orientation and to redress any biomechanical imbalance that is felt to be contributing to hip instability. Again, clinical and surgical experience is important in this challenging situation. Unfortunately, the results of revision for instability are not always as consistent as we would hope for our patients.
Fracture around the hip replacement
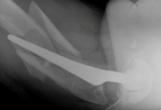
Other, perhaps less common, causes of patients requiring hip revision surgery include fracture around the components as a consequence of a fall or traumatic injury. Again, this is more common when in association with a degree of wear-related loosening of the components and bone damage occurring both as a cause, and indeed consequence, of that loosening.
Unfortunately, periprosthetic fracture can also occur in a hip replacement that has previously functioned normally.
Managing this distressing complication is challenging. Decisions are based on the location of the fracture relative to the implants, the pre-fracture function of the hip replacement (whether there was evidence of loosening of the implants) and on the quality of the bone around the implant. The options are to reduce and fix the fracture around the components or to consider removing the implants and replacing them with revision components. This decision is based on experience and will typically be taken following discussions between surgeons with both trauma and revision experience.
Other, more unusual, reasons for hip revision include:
- Very rarely the metallic components themselves break and require revision
- Failure of the soft tissue repair around the hip replacement that can result in weakness or abnormal movement
- Surgery, with or without component revision, should bone form in the soft tissue scar tissue around the replacement causing restricted movement
- Surgery to release soft tissues if they catch around the edges of the metallic components
- Revision surgery can also be required if there is a significant and/or troublesome leg length inequality after surgery
It is important that any decision to consider revision is made only after significant targeted investigation, ideally with a definite understanding of the reasons behind any failure of the replacement, with a very defined understanding of what revision procedure is to be performed, what the expectations are for that revision as well as the specific risks and concerns. Blind exploration of a painful hip replacement without a defined and understood indication for a patient’s symptoms is rarely a sensible option.
With all of the above potential complexity, any decision to proceed with revision hip arthroplasty surgery should be made following discussions within a Multi-Disciplinary Team (MDT) meeting, such as the pioneering East Midlands Specialist Orthopaedic Network (EMSON) which I was involved in setting up in 2015 in Nottingham. Our collective, supportive and cohesive approach process has been presented and recognised worldwide as a blueprint option for how this MDT process can be run.